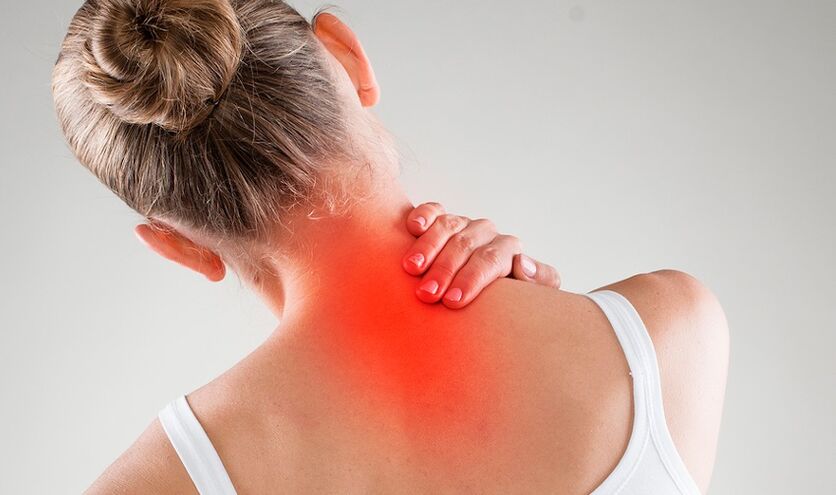
Osteochondrosis of the cervical spine or cervical osteochondrosis is a disease of degenerative-dystrophic genesis that affects the intervertebral discs and cervical vertebrae with the formation of protrusions and intervertebral hernias, which eventually leads to dysfunction of the spinal cord and is often the cause of the patient's disability.
Features of the structure of the cervical spine
The vertebrae are the bones from which the vertebral column is built. Each vertebra has a body, which carries the entire load, the vertebral arch, transverse and spinous processes.
The vertebral arches of the vertebrae form the vertebral canal through which the spinal cord passes. The processes of the spine are designed to anchor the muscles of the back.
There are also anterior and posterior ligaments that connect the vertebrae together.
The intervertebral disc is a rounded flat structure that consists of an annulus fibrosus and a nucleus pulposus, the main function of which is shock absorption. The intervertebral discs are located between the vertebrae.
The facet joint is a movable connection of the processes of two adjacent vertebrae. The facet joints provide flexibility to the spine.
Intervertebral foramen are foramina that are formed by structural elements (legs, articular processes) of two adjacent vertebrae and are intended for the exit of the root nerves of the spinal cord.
There are paravertebral muscles to support the spine and its various movements.
The cervical spine is the uppermost and most mobile part of the spine, which consists of seven vertebrae and has a C-shape due to its forward bend (cervical lordosis).
All head movements - tilt, turn, circular, are provided by this part of the spine.
Interesting!In addition, the cervical spine is the most traumatized part, since the cervical vertebrae have low strength and weak muscular apparatus, in comparison with others.
For the same reason, osteochondrosis of the cervical spine often occurs.
Prevalence of cervical osteochondrosis
Osteochondrosis of the cervical spine affects the working-age population over the age of 30. This disease is more common in women than in men.
According to the World Health Organization, 40-90% of the world's population suffers from osteochondrosis.
Important!Every second patient with osteochondrosis has dystrophic and degenerative changes in the spine in the cervical spine.
Causes of osteochondrosis of the cervical spine
Osteochondrosis can be called a tribute for the ability of a person to stand and walk on two legs. This opinion is confirmed by the fact that not a single animal that walks on four legs suffers from osteochondrosis.
Despite the availability of modern methods for diagnosing diseases and deep knowledge of human anatomy and physiology, it has not yet been possible to establish the specific causes of osteochondrosis.

But reliable factors are known that lead to degenerative-dystrophic changes in the spinal column. These include the following:
- insufficiently mobile lifestyle of a person, which leads to a weakening of the muscular apparatus of the back. Often, office workers, cashiers, salesmen, and drivers suffer from osteochondrosis;
- hard physical labor;
- mechanical injury to the back;
- genetic predisposition to osteochondrosis;
- overweight and obesity;
- neuropsychic stress;
- improper workouts in the gym;
- beriberi, micronutrient deficiency, metabolic disorders;
- improper nutrition;
- the presence of diseases of the kidneys, digestive and endocrine systems;
- infectious diseases;
- frequent hypothermia of the body;
- congenital and acquired immunodeficiencies.
Pathogenesis (development mechanism) of cervical osteochondrosis

Almost all contributing factors in the development of osteochondrosis lead to spasm of the back muscles. In turn, muscle spasm disrupts the blood supply and metabolism of the bone tissue of the vertebrae and intervertebral discs.
Thus, dystrophic changes occur, in other words, drying out, dehydration and loss of elasticity of the vertebrae and intervertebral discs.
Further stress on the spine leads to flattening, protrusion (protrusion beyond the annulus fibrosus) of the intervertebral discs.
No less important in the pathogenesis of cervical osteochondrosis is the load from holding and moving the head.
The load on the cervical vertebrae is enormous, because the average weight of the head is 3-5 kg, and their bone tissue, unfortunately, is fragile and thin.
Also, the development of osteochondrosis is facilitated by technical progress - smartphones, tablets, e-books, if stooping while using these gadgets.
The intervertebral discs cannot efficiently perform amortization of the spinal column, therefore, compensatory mechanisms are triggered.
Important!One of these mechanisms is the proliferation of osteophytes and the development of spondylosis.
False joints can also form along the back surface of the vertebrae of the cervical spine - uncovertebral arthrosis.
All these processes eventually lead to a decrease in cervical lordosis (hypolordosis), protrusions and intervertebral discs, which sooner or later become the main cause of a person's disability or require urgent surgical treatment.
The pathogenesis of cervical osteochondrosis can be divided into four stages:
- The onset of instability of the cervical vertebrae;
- The formation of protrusion of the intervertebral discs, a decrease in the intervertebral fissure, the beginning of the destruction of the annulus fibrosus, which leads to pinching of the nerves, which manifests itself in pain in the neck;
- The annulus fibrosus is destroyed completely and the nucleus pulposus extends beyond its borders, thus, an intervertebral hernia is formed and the spine is deformed;
- Stage of disability. The vertebrae grow together. It is difficult for patients to move. Sometimes the condition may improve, but not for long.
Symptoms and syndromes in osteochondrosis of the cervical spine
The main symptoms of cervical osteochondrosis include the following:
- persistent neck pain of a throbbing or aching nature, which can spread to the occipital region of the head, eye orbits, ears and shoulder girdle;
- pain in the upper limbs, which increases when they move;
- stiffness of movements of the upper limbs, violation of their sensitivity (tingling, burning, numbness), weakening of strength in the muscles;
- morning stiffness in the neck;
- soreness in the cervical spine when moving the head;
- periodic dizziness with cervical osteochondrosis, darkening in the eyes, loss of consciousness with sharp turns of the head;
- sensation of tinnitus;
- hearing and vision impairment;
- feeling of numbness and tingling in the tongue;
- cardialgia (pain in the heart), sometimes cervical osteochondrosis is mistaken for acute coronary syndrome. The difference is the lack of effect from nitrates;
- due to microcirculation disorders and tissue oxygen deficiency, connective tissue proliferates in the cervical spine, the so-called "withers".
All symptoms of cervical osteochondrosis can be grouped into the following syndromes:
- reflex;
- radicular;
- radicular-vascular;
- spinal compression;
- cerebral.
Reflex syndrome consists of cervicalgia - intense pain in the neck, due to which the patient is forced to fix the head and strain the neck muscles.
Feeling the spinous processes, paravertebral points and intervertebral discs brings and / or increases pain.
Also, reflex syndrome is characterized by pain in the upper limbs, occipital or temporal regions of the head.
Radicular syndrome is a combination of sharp acute pain that increases with head movements and arises from pinching of nerves in the intervertebral foramen.
The radicular-vascular syndrome is characterized by vegetative-trophic disorders in the form of humeral-scapular periarthritis.
The patient is worried about pain in the shoulder joint, stiffness of movements, impaired sensitivity of the skin, swelling of the hand and wrist joint. Also, the patient cannot bring his hands back.
Spinal compression syndrome occurs due to compression of the spinal cord and its vascular apparatus. Herniated discs, osteophytes, thickening of the yellow ligament can lead to this.
Interesting!Patients have pain in the cervicobrachial region, flaccid paresis of the upper extremities and spastic paresis of the lower extremities, impaired sensitivity.
Cerebral syndrome with cervical osteochondrosis combines several such syndromes:
- diencephalic syndrome - increased irritability, neurasthenia, general weakness, insomnia, absent-mindedness. In severe cases, there is anxiety, numbness of the upper and lower extremities, increased sweating, chills;
- posterior cervical sympathetic Barre syndrome or "cervical migraine" - intense headaches, as with migraine in one half of the head against the background of dizziness, visual and hearing impairment, feeling of numbness in the hands.
- syncope syndrome - fainting with a sharp turn of the head;
- vestibular-stem and cochlear-stem syndromes - dizziness, unsteadiness when walking, nausea and even vomiting;
- visual impairment syndrome - visual impairment, visual impairment, flashing "points", "flies" in front of the eyes.
Diagnostics of the osteochondrosis of the cervical spine
As with any diagnosis in medicine, the diagnosis of osteochondrosis of the cervical spine is established on the basis of the patient's complaints, medical history, examination and auxiliary research methods.
In addition to clinical examination, the patient must undergo the following methods:
- X-ray of the cervical spine;
- Computed tomography of the cervical spine;
- Magnetic resonance imaging of the cervical spine;
- Doppler ultrasound examination of the vessels of the neck;
After diagnostic measures, the doctor chooses the treatment tactics based on the results of the diagnostics and analyzes.
Treatment of osteochondrosis of the cervical spine
Treatment of osteochondrosis of the cervical spine consists in the elimination of radicular syndrome and the removal of the inflammatory process.

In the acute period of the disease, you must adhere to strict bed rest. The soft mattress should be replaced with a hard one, or a wooden shield should be placed over it.
Drug therapy for cervical osteochondrosis is carried out using the following groups of drugs:
- non-steroidal anti-inflammatory drugs;
- drugs of the chondroprotective group;
- pain relievers and anti-inflammatory gels and ointments;
- vitamin preparations - ascorbic acid, retinol acetate, tocopherol acetate;
- calcium preparations;
- drugs that improve microcirculation in tissues;
- muscle relaxants.
Treatment of cervical osteochondrosis includes the following methods:
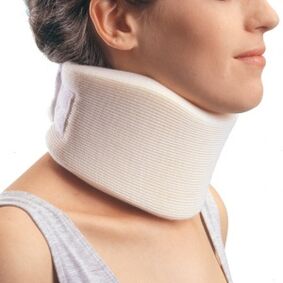
- wearing a special collar around the neck, which not only relieves the load from the neck, but also limits movement;
- stretching with a glisson loop - the patient's head, who is lying on the bed, is fixed with a glisson loop, and the head of the bed is raised by 20-30 cm. This procedure relaxes the muscular corset of the spine, increases the intervertebral fissures, releases pinched nerves;
- manual therapy for cervical osteochondrosis should be carried out only by an experienced manual therapist. Manual therapy is performed using relaxing and segmental massage techniques, mobilization, which restores damaged joint functions, and manipulations to restore full range of motion in the joints.
- physiotherapy methods for osteochondrosis of the cervical spine - diadynamic therapy, electrotherapy, laser therapy, shock wave therapy, balneotherapy, treatment with ultrasound and ultraviolet rays, magnetotherapy and other methods.
- Physiotherapy for cervical osteochondrosis includes exercises to strengthen the muscle corset. Physical exercise is suitable not only for the treatment of osteochondrosis, but also for prevention. They can be done before going to bed at home, at the gym, at work and school during breaks.
Surgical treatment of cervical osteochondrosis
Treatment with surgical methods is indicated for severe radicular syndrome, which cannot be relieved by medication, with an increase in impairment of the motor and sensory functions of the upper limbs, as well as with compression of the spinal cord.
Important!Operations to remove herniated intervertebral discs and osteophytes are widely used.
Prevention of osteochondrosis of the cervical spine

- healthy sleep on an orthopedic mattress;
- using a low pillow;
- visit the sauna or bath regularly. Steam perfectly relaxes the neck muscles;
- you need to take a hot shower daily for at least 10 minutes;
- going in for sports, gymnastics, walking. Swimming, yoga, Pilates are great for this;
- all head movements should be accurate, without sharp turns;
- correctly distribute the load on the spine during physical labor and sports;
- take breaks and warm-ups during sedentary work;
- keep the correct posture while sitting at a table or computer;
- chairs and a table should be appropriate for your height.



















